

Bunions
A swelling or enlargement of the joint of the big toe is commonly referred to as a bunion deformity. The cause of a bunion is genetics, it is usually inherited. A parent or a grandparent may have suffered with a similar affliction. However, it can become irritated by a tight or inappropriate shoe. The predisposition for bunions is usually in the form of a foot that flattens too much when walking. Excessive dropping of the arch then places more weight on the big toe causing arthritic damage and bunion deformity. It should be noted that patients with a high arch can also have bunions. The question is less that of how high the arch is, but how much it falls. Patients usually present to our office with pain to the bunion site caused by rubbing or irrigation of the bone enlargement on shoe gear. This pain can range from slightly annoying to downright debilitating.
Several options exist for treating a bunion deformity. Surprisingly, most bunions can be treated conservatively. These conservative treatments include custom made orthotics to offload the area, change in shoe gear, cortisone injections. In some cases when conservative treatment has failed, surgical options may be utilized. Surgical procedures vary based on the severity of the deformity. Dr. Brucato has been extensively trained in minimally invasive bunion surgery which is the use of very small incisions and instrumentation to provide a more aesthetic result and faster return to work and activity.

Calluses
Although many people consider calluses to be a simple skin problem, it is actually an indicator of bone problems. In the foot, calluses are typically seen on the heels, balls of the feet, and on the outer side of the big toe. Calluses have their own nerves and sacks of fluid that act as cushioning, which can cause pain over time.

Hammertoes
Curling of the toes as they grip the floor, bending the the proximal interphalangeal joint is called a hammertoe. Hammertoes can be caused by a number of etiologies. The most common is a genetic disposition to a flattening arch. As the arch flattens, the toes tend to grip the supporting surface. Measurements of the degree of the flattening can often bet achieved with the use of diagnostic ultrasound and sometimes with evaluation of gait pattern. If hammertoes are noted to be caused by a flattening of the arch, orthotics or customized supports can sometimes be used to prevent a further progression of the deformity. As hammertoes progress, the joints of the toes have uneven pressure placed upon them. This causes bone spurs to develop. These spurs then put pressure against the skin and the skin rubs against the shoe or another toe. In order for the skin to protect itself from the pressure, it then thickens. When the skin gets too thick, it forms a corn or callous. Many times these are associated with pain and in some cases ulceration. Additionally, the rubbing of the corn on the toe can cause inflammation and swelling to become trapped in the toe joint.
Conservative treatments for hammertoes include changes in shoe gear, reduction of an associated corn or callus, custom molded orthotics, cortisone injections into the joint to alleviate inflammation and hyaluronic acid injections to shrink the thickening of the joints in the hammertoe. If these treatments fail, typically the only way to permanently fix a hammertoe is with surgical correction. We recommend exhausting all treatments prior to discussing the surgical procedure.
Dr. Brucato performs a variety of different hammertoe procedures including minimally invasive flexor tenotomies which can be done in the office as well as straightening of the hammertoe utilizing an absorbable implant (no pins sticking out, no metal stuck in toe).

Diabetic Foot Care
Diabetes is a chronic disease causing high blood glucose (sugar) levels. Diabetes also weakens your immune system, making it more difficult for your body to fight off infections, which can, in turn, damage your nervous system. This damage can affect the ability to feel sensations in your feet.

Warts
Plantar warts are caused by a virus that is found in the environment. Your body doesn't recognize the virus and forms a hard callus over the top of it. They do require treatment because they are contagious and tend to spread with time. Dr. Brucato performs painless treatment in the office for these warts and for the most difficult cases, she has the ability to laser them out.
We offer two types of laser treatments:
Our YAG in-office laser machine
Dr. Brucato can do laser removal in OR which is post dye laser

Plantar Fasciitis
Plantar fasciitis is the most common condition that causes heel pain. This condition occurs when the long fascia ligament along the bottom of the foot develops tears, resulting in pain and inflammation. This ligaments main function is to stop your arch from coming down too far, and assist it in coming back up. If your archy begins to come down too far or “fall”, this ligament will tear. Many times pain in the heel is greatest in the morning or are sitting for awhile. When you are off the ligament it begins to heal and when we place pressure on it, it tears. Pain usually decreases as the tissue warms up, but may easily return again after a long period of standing or weight bearing or physical activity. In most cases, plantar fasciitis does not require surgery to stop the pain and reverse damage. Conservative treatments are usually all that is required. However, every person’s body responds differently and the goal is to prevent arthritis in other joints as well as alleviate the heel and foot pain. Another problem is a change in your walking in order to counteract the pain during movement. As a result, these involuntary changes in the mechanics of the foot, knee, hip or back pain can also develop.
Initial evaluation may require x-ray or diagnostic ultrasound which can differentiate between a neuroma, stress fracture, tumor, tendonitis, etc. Should diagnosis of neuroma be made, further evaluation will include a taping of the arch for 24 hours. This taping will assist the doctor in understand both the severity of your condition and the most appropriate treatment course. Treatment course will depend in your response to the taping test. The following are potential options: 95% improvement usually will require custom orthotic, possible physiotherapy done in the office. 80-95% improvement usually requires 1 cortisone injection and custom orthotics. 50% and above improvement usually requires 3 sets of cortisone injections, orthotics, and physiotherapy. After these treatments, a delayed stretching routine is prescribed along with possible night splints. If the pain is worse with the taping, an MRI is ordered to rule out any other injury and the foot is immobilized in a soft cast.More invasive procedures to treat plantar fasciitis are usually sought only after other treatments have failed to produce favorable results. These more aggressive treatments include PRP injections, amniotic membrane injections, and extracorporeal shock wave therapy (ESWT). ESWT is a treatment where sounds waves are sent through the damaged tissue in order to encourage healing. In most cases, heel spurs can be treated with these simple methods. If more conservative methods fail to produce positive, long lasting results, surgery may be considered to remove the spur or to release tension in the plantar fascia to stop further damage.

Heel Pain
Heel pain is one of the most common complaints from patients. While heel spurs may or may not show up on an x-ray, the spurs themselves are a result of the actual problem: plantar fasciitis.

Ankle Pain
Ankle sprains occur when the ankle is twisted or forced in a way that stretches or tears one or more ligaments. The severity of the injury depends on if the ligaments are stretched, partially torn, or fully torn. Symptoms of an ankle sprain include pain, bruising, swelling, stiffness, and difficulty walking.

Flat Feet
A common condition of the foot structure, flat feet, is caused by an undeveloped arch of the foot. While infants and toddlers lack arches in their feet, the structure continues to develop through adolescence and is fully formed by adulthood.

Athlete's Foot
Athlete’s foot is a contagious fungal infection that mostly affects the feet, with the potential to spread to toenails and hands. The fungus thrives in warm, humid, and dark environments, which makes athletes more prone to the infection. Communal showers, swimming pools, and locker rooms are hotbeds for the bacteria.

Achilles Tendonitis
The Achilles tendon is the largest tendon in the body, joining the lower portion of the calf to the heel bone. Although it is able to withstand forces of around 1,000 pounds, it is the most frequently ruptured tendon in the body. Typically, injury of the Achilles tendon is caused by athletic activities.

Neuromas
A neuroma is a pinched nerve in the front of the foot often caused by your foot shape. It is made worse by walking barefoot or narrow shoes. A neuroma can cause a variety of symptoms including pain, burning, numbness, tingling, or having the sensation your sock is balled up under your toes. The first line treatments are cortisone injections and/or custom molded orthotics. A more aggressive approach includes deadening the nerve with a series of alcohol sclerosing injections and the last resort is surgical excision.

Toenail Fungus
Fungal nail infections require a process of treatments along with a continual effort to prevent it from recurring. Keeping the infection under control can include thoroughly washing and drying feet, applying anti-fungal cream, not sharing nail clippers or shoes/socks, wearing dry cotton socks and changing them often, wearing dry shoes, and using shower sandals in wet, public places.
Treatment:
Dr. Brucato has a special laser in her office to kill the fungus living in the nail bed underneath the nail and is an entirely pain-free treatment. The laser has great results but unfortunately is not covered by insurance. However, you will find we have one of the most affordable pricing available in New Jersey.

Neuropathy
As a result of damaged peripheral nerves, peripheral neuropathy can occur causing symptoms like weakness, numbness, burning, and tingling in the hands and feet as well as other parts of the body. Traumatic injuries, diabetes, and even some exposure to toxins can cause peripheral nerve damage.
Dr. Brucato performs a variety of treatments for neuropathy including physiotherapy treatments such as electric stimulation, laser, and ultrasound treatments. In-office B-12 injections have also helped our neuropathy patients greatly. In the worst cases, Dr. Brucato performs surgical intervention which is triple nerve decompression to release pressure on the main nerves to the foot. This is also known as the Dellon procedure.
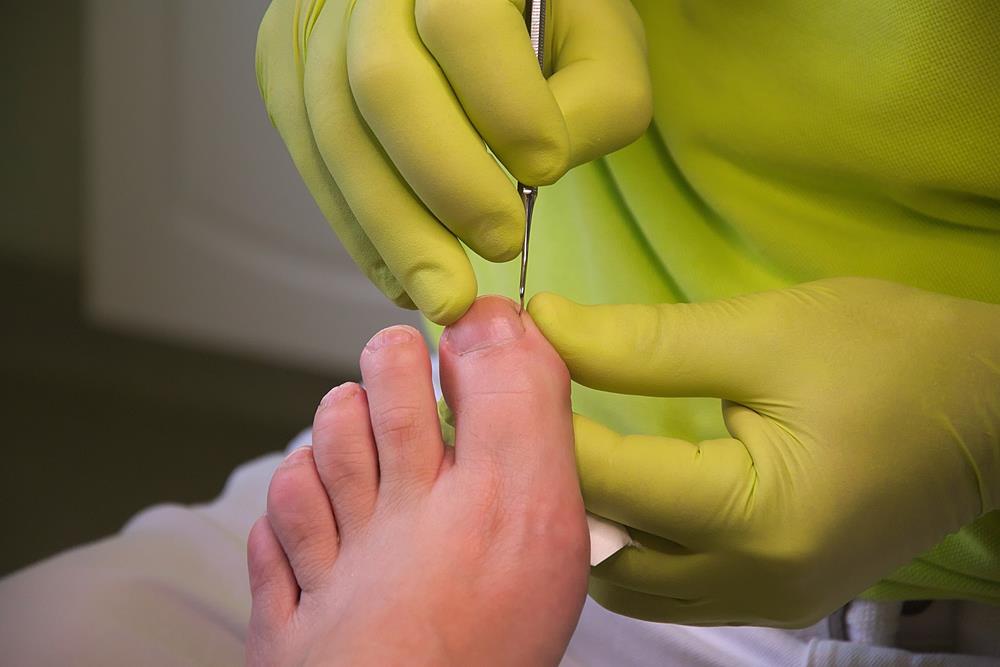
Ingrown Toenails
An ingrown nail is a nail that curves into the skin. It may or may not be painful, and may or may not cause infection. An ingrown nail that causes infection or inflammation is called a paronychia.
Causes:
- Trauma, or any damage to the nail or the nail bed can result in ingrown nails
- Shoes, especially narrow shoes that are too small and squeeze the nail into the skin
- Fungus causes changes in the shape of the nail and the nail bed, sometimes resulting in
ingrown toenails - Genetics
- Cutting the nails too short. Always avoid cutting the nails short and deep into the corner
- Women following childbirth are more prone to ingrown nails
- Pedicures
Treatment:
May be as simple as reducing the end of the ingrown nail. If the nail is deeply ingrown, surgical removal of the offending nail border and treatment of the nail root so that this situation does not recur is the usual treatment of choice.

Sever's Disease
Calcaneal apophysitis also known as Sever’s disease occurs most commonly in males between the ages of 10-13. It is also seen to a lesser degree in females. Sometimes this condition is known as “growing pains”. The pain is usually located in the back of the heel, but can also be noted on the bottom as well. Pain is usually related to increased activity and is most often associated with a specific sport. The patient will often relate pain upon running or doing that activity. Pain, many times, feels better when doing the activity but increases once the activity has stopped. As an example, a child may be able to play soccer with no problem, but once the game is over, has difficulty walking. Pain can range from mild to debilitating. The reasoning behind decreased pain with increased activity relates to a tear of the tendon on a very small level. When running, micro-tears develop in the tendon and this is attached to the growth plate. Once torn, these tears are usually non-painful. When the activity ceases, they begin to heal. Pain once again occurs as these re-tear.
Cause:
The cause of the problem is that the growth of the long bones of the leg (the tibia and the fibula) occurs at a faster rate than the Achilles tendon. As the bone grows in length, the tendon struggles to keep up with the growth. Extra pressure is then placed on the apophysis or growth plate of the heel bone called the calcaneous.
Treatment:
Evaluation usually includes ultrasound exam as well as radiographic analysis. Assuming that these indicate apophysitis, a low dye taping is applied to the bottom of the foot. This taping is used to take the pressure off the apophyseal plate. The patient is asked to wear this for 24 hours. The patient’s response to the taping would then determine the treatment. Should the taping afford 95-100% relief of discomfort, customized orthotic treatment would probably be necessary as well as some type of temporary support. Should the patient relate a history of 50% or greater relief of discomfort, immobilization may be used as well. This immobilization would most likely take the form of a soft cast for 3-4 days. Should the pain relief with the taping be less than 50%, a longer term immobilization may be utilized with a fiberglass cast or Cam walker. In all cases, the usually long term treatment for this situation will be a biomechanical orthotic even if it is utilized for 6 months to a year until the rapid growth of the long bones ceases. Calcaneal apophysitis is a very treatable condition. If not treated, the inflammation in the growth plate could cause weakening and progress to a fracture of the growth plate. Long term prognosis for an aggressively treated apophysitis is excellent.

Limb Length Discrepancy
Our practice has biomechanically trained physicians to properly measure a limb length discrepancy. Oftentimes we are able to add an lift to orthotics to even the patient out. This can also help patients with scoliosis.
